ICSI
ICSI – Intra-Cytoplasmic Sperm Injection (test tube fertilization with microinjection of sperm)
Conventional IVF and ICSI
Basic therapy of ICSI is IVF. The only difference from IVF is that in this case we do not add 100,000 sperm to each egg, but we inject a single sperm into one egg.
Procedure
1. Drug pre-treatment
In conventional IVF, a drug pre-treatment is used to create optimal hormonal conditions and a relatively high number of eggs. For this purpose, usually 150-225 I.U. FSH (Gonal-F or Puregon) or a FSH/LH mixture (Menogon) is injected daily, subcutaneously (under the skin). Various drugs are also needed to prevent premature ovulation (Synarela spray; Zoladex, Enantone, Dekapeptyl).
When enough follicles (egg sacs) have grown, the so-called “ovulation injection” (Brevactide, Pregnesin, Ovitrelle) is administered to complete the egg maturation phase. With the help of a follicle puncture, several oocytes are now usually collected.
2. Egg collection
Vaginal follicular puncture under ultrasound guidance is usually done under a short anesthesia 32 to 36 hours after the HCG injection.
In this procedure, a puncture needle is passed through the wall of the vagina to the ovary using an ultrasound probe. There, one follicle (egg sac) at a time is then punctured. The fluid is aspirated and given directly to the biologist so that it can be immediately determined if there is an egg in it.
3. Fertilisation
One sperm is injected into each egg in the laboratory using an elaborate microscope. The dishes are then “incubated” (cultured) overnight in an incubator.
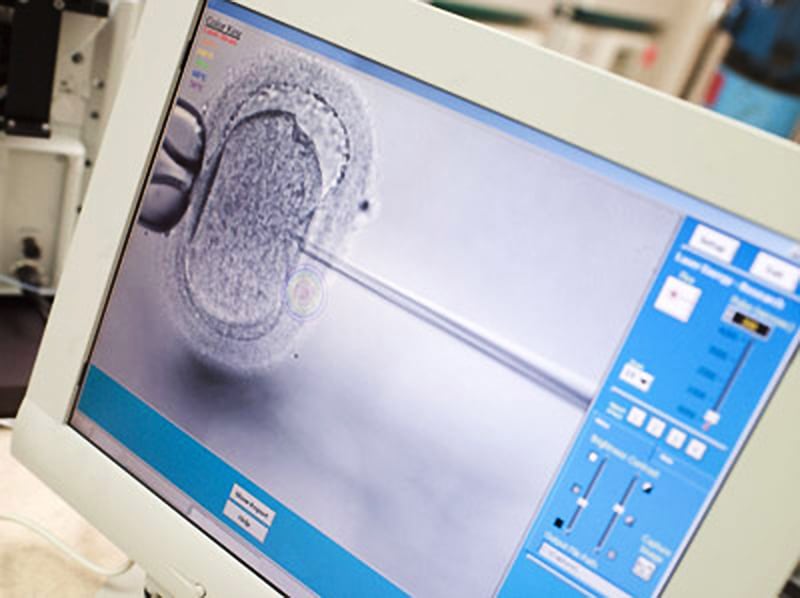
… then a glass capillary is used to inject the sperm directly into the egg.
19-21 hours later, after determining how many eggs have reached the so-called pronucleus stage (PN stage-pro nucleus), it is necessary (at least in Germany) to select which PN stage cells (max. 3) should complete the fertilization process. The pronuclei contain the chromosomes of the egg cell and the sperm cell respectively.
On the 2nd or 3rd day after sperm addition, when one or more embryos have developed, the embryo(s) are transferred to the uterine cavity. Transfer on the 5th day is also possible and useful if one or more blastocysts have developed by then.
More information about blastocyst transfer.
4. Embryo transfer
Embryo transfer is performed on the 2nd, 3rd or 5th day after sperm addition. In this procedure, a catheter is inserted into the uterine cavity without causing any pain, possibly under ultrasound control. The embryo(s) is/are then carefully deposited there. In preparation for this transfer, the woman may take medication that calms the uterine muscles. By adding progesterone (luteal hormone: Crinone gel, Utrogest) , optimal mucosal conditions for implantation (implantation) of the embryo should be achieved over the next 14 days.
In the period after the embryo transfer, excitement and too much activity should be avoided, as well as circulatory stress, e.g. through sports and strong temperature increases, e.g. sauna visits, hot tub baths. Otherwise, there are no special recommendations to be made. Sex also tends to have a positive effect.
12 to 14 days after fertilization, a urine pregnancy test or a blood test can determine whether the woman is pregnant.
Again, the basic treatment can be individualized. The different types of IVF, NC-IVF, Mini-IVF™ and conventional IVF are described elsewhere.
